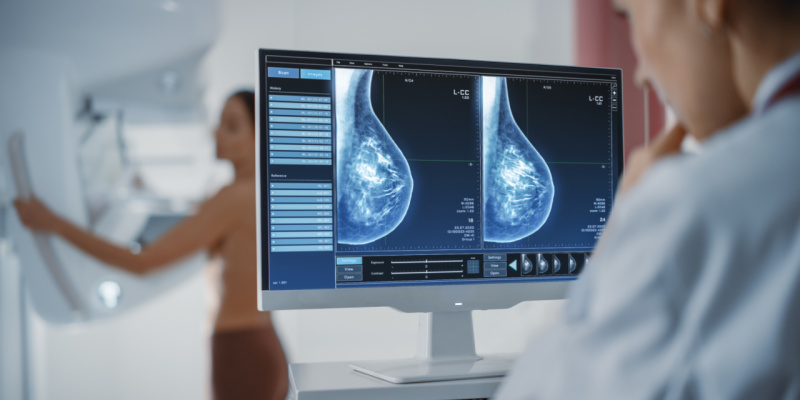
By Sue Sveum
We hear a lot about early detection — and there’s no doubt that it plays a very important role in identifying and treating the early stages of breast cancer.
But what some women may not realize, is that anyone — even young women or those with no family history — can get breast cancer.
That’s why it’s so important to know your own body – and contact your provider immediately if you notice anything that seems unusual. We asked a few SSM Health providers and two of their cancer patients to share their stories – and a little advice – with us. The good news? The sooner you act, the better your chances of a positive outcome.
Living with Breast Cancer
According to Dr. Dana Henkel, screening is still the best way to detect cancer early — many times long before any other signs or symptoms like a lump would appear. “But some women worry about pain, feel they’re too busy or fear finding something they don’t want to deal with,” explains Henkel. “If they have no family history, they may simply think ‘it’ll never happen to me.’”
Maggie Huff, an SSM Health mammographer, agrees, adding, “An abnormal result after your screening mammogram doesn’t necessarily mean you have breast cancer.” The radiologist may want additional images or an ultrasound, but usually these additional images will show normal breast tissue.
“Getting a yearly mammogram isn’t going to prevent breast cancer,” Huff adds, “but will help detect it at the earliest stages — giving you more treatment options with a better success rate. It can literally save your life.”
And for those worried about pain, she points out how many uncomfortable things women choose to do regularly, including waxing, plastic surgeries, dental procedures — and even working out.
But what about those younger women who haven’t reached the recommended age for screenings yet?
Amanda was young and healthy and just 28 years old when she noticed discharge from her right nipple. “I knew something wasn’t right,” she says, “so I called my primary care doctor right away.” A blood test came back normal, but a couple ultrasounds and a biopsy revealed a quarter-sized tumor — and the diagnosis of triple negative breast cancer.
“Triple negative is an aggressive cancer that tends to grow and spread quickly,” explains Henkel.
“Unfortunately, there aren’t good options for ‘targeted’ treatments, so oncologists use chemotherapy to try to eradicate the cancer.”
And that’s exactly what happened in Amanda’s case. “From there, things moved pretty quickly,” explains Amanda, whose treatment started out with six months of chemo followed by a double mastectomy. “The good news is that the chemo completely eradicated my cancer,” she says.
“But I decided to go ahead with a double mastectomy anyway, as a precaution — and to keep everything looking more even.” She had reconstruction surgery a couple months later.
“The collaboration between the entire team at SSM Health was great,” stresses Amanda. “Everyone had my best interests at heart and was on the same page throughout the whole process.”
Dr. Henkel also referred her to a fertility specialist. “I was so focused on the diagnosis, that having children someday was something I’d never thought about,” says Amanda. “Although it was a tight window to get it done quickly before starting chemo, I was able to save 25 eggs, although I didn’t end up needing them.”
Your Body, Your Health
Although women with breast cancer may have a lot in common — and can certainly find comfort in the support they get and give to one another — each breast cancer is a little different.
Like many other women during the pandemic, Mary’s annual mammogram got pushed to the back burner, so it was a relief when it came back normal. But four months later, she noticed blood around her nipple at night and realized something was wrong. “It wasn’t just a drop,” she says. “It filled an entire Kleenex.” Like Amanda, she immediately turned to her primary care provider, who assured her that doesn’t always mean cancer. But in her case, it did.
Starting with the diagnostic stage, Mary met with Cindy Vickerman, a nurse navigator. “She set up my procedures, called me with the results — and suggested that I not read the results when they first pop up on MyChart,” Mary laughed.
“My role as a nurse navigator is to focus on education and reassurance through the biopsy process,” explains Vickerman. “But I always let patients know they should keep my contact information handy — and can always call me for support or questions along the way.”
Vickerman says she believes knowledge is power when it comes to beginning a journey through breast cancer. “It’s so important to ask questions and have all of the information you need to make sound decisions about your own health and treatment,” she stresses. “No woman’s journey looks exactly the same [as another], but it’s important to be active in the shared decision-making with your physicians.”
For Mary, another mammogram, an ultrasound, an MRI and biopsy revealed that she had ductal carcinoma in situ (DCIS) as well as multiple larger tumors. Due to the size and extent of her cancer, she underwent a mastectomy, followed by chemo and then radiation.
For patients like Mary, postmastectomy radiation therapy directed to the chest wall and lymph nodes is often used to decrease the risk of a recurrence — and to improve overall survival, according to Dr. Michelle Mackay, Mary’s radiation oncologist. “Our multidisciplinary team of doctors and other medical professionals work together to design the optimal treatment plan for each individual patient.”
“Radiation recommendations are based on the diagnosis and stage,” she explains. “But the patient always has a choice in their treatment plan — and ultimately, they decide how they wish to proceed.”
Mary welcomed the team collaboration. “Once I knew we had a plan in place, I felt better knowing we could move forward,” she says. “Everyone did a great job — and kept me in the loop so I felt comfortable.”
She describes radiation as a strange experience that you can’t feel or smell, but you notice over time. Of chemotherapy, she confides it’s pretty disturbing to see your hair fall out. Her solution? Have her stylist shave it off. “As upsetting as losing your hair is, after a while you get used to it,” she says. “It’s just hair. But I’m still here.”
Mary adds that looking too far ahead can be overwhelming. “I’d tell other women, just take one step atatime.”
Mackay stresses that while she advocates mammography as the gold standard for early detection, it’s also important to know your body and seek further evaluation if something changes. “Mary’s mammogram was normal,” she says, “but fortunately when she noticed a change in her breast, she got it checked out.”
Henkel agrees. “Pay attention to your body’s signs that something might not be right,” she stresses. “Recognizing something different about your breasts — whether it’s a lump or nipple discharge — and seeing your physician, is key to sorting through those signs and correctly diagnosing the problem.”
“My diagnosis was very scary,” recalls Amanda, whose grandmother died of breast cancer at a young age. “And we had recently lost my father to brain cancer. So, it was extra scary — because I decided I was going to have to be the first person in the family to beat this.”
It was a rough year, but there is a happy ending for Amanda, who met her husband while she was undergoing treatment. “We started dating when I had no hair,” she laughs. “He’s amazing.” Three years later she’s cancer-free, happily married, and pregnant with the couple’s first child. All thanks to seeing her doctor when something didn’t seem right.
My Breast Cancer Story
By Sue Sveum
I’m no stranger to the importance of breast cancer detection after working for the American Cancer Society and writing about it for SSM Health. With no family history of cancer and a couple decades’ worth of mammograms under my belt, I never expected to experience it myself — but I did.
I’d headed to my annual mammogram with the nonchalance of going to the hair salon. Even after I was called back for a magnified image, I wasn’t concerned. A couple suspicious spots led to a biopsy, but hey, the brochure said 80% of women who get a biopsy don’t have cancer. But when the nurse navigator called while I was driving and gently asked if she should call back, it suddenly became real — I had cancer.
I was diagnosed with ductal carcinoma in situ (DCIS). Fortunately, DCIS is an early-stage cancer still contained in the milk ducts and not invasive. I was immediately assigned a nurse navigator (Cindy Vickerman), a surgeon, (Dr. Dana Henkel), an oncologist and radiation oncologist — all of whom were knowledgeable, professional and caring (a quality I can’t stress enough!). Since cancer was still detected after an initial lumpectomy, I had a mastectomy, which came back clear — meaning I wouldn’t need chemo or radiation.
A breast cancer diagnosis isn’t something anyone wants to hear. But in my case, there was no lump — and I wouldn’t have found it on my own. I will be forever grateful for routine mammograms and early detection.
If you haven’t already, please see your provider for an annual physical — and if recommended, schedule your mammogram today!